On this page
What is Exercise-Induced anaphylaxis?
Exercise-induced anaphylaxis (EIA) is a condition in which anaphylaxis (a severe allergic reaction) occurs either during or after exercise.
EIA may occur alone or with cofactors or triggers (such as food or medication).
When EIA is associated with food, it is known as Food-Dependent Exercise-Induced Anaphylaxis (FDEIA). With FDEIA, the food trigger (most commonly wheat) can be safely eaten if there is no activity.
What defines ‘activity’ will vary between individuals, but for some, even unpacking shopping will be enough to cause a reaction if the trigger food is consumed.
NOTE: Exercise (being physically active) can worsen an allergic reaction in anyone who is at risk of anaphylaxis. This response to activity/exercise is NOT the same as a diagnosis of Exercise-Induced Anaphylaxis (EIA) or Food-Dependent Exercise-Induced Anaphylaxis (FDEIA).
Cofactors for EIA
- EIA may occur on its own without cofactors but cofactors such as food or medication are more commonly needed to trigger symptoms.
- The vast majority of those with anaphylaxis occurring during exercise are allergic to food eaten in the previous 6 hours, which is called Food-Dependent Exercise-Induced Anaphylaxis (FDEIA).
- The food does not normally result in an allergic reaction when eaten alone but can trigger anaphylaxis when the food is eaten up to approximately 6 hours before exercise or sometimes even 4 hours after exercise.
- The relationship to non-steroidal anti-inflammatory drugs (NSAIDs):
- NSAIDs and EIA: Anaphylaxis may occur when a NSAID, such as aspirin or ibuprofen, has been taken prior to exercise.
- Food, NSAIDs and FDEIA: The combination of a trigger food and NSAIDs prior to exercise has the potential to trigger FDEIA. In some individuals, simply taking NSAIDs if you have consumed the trigger food can result in an allergic reaction.
Other cofactors may lead to symptoms being triggered with less exercise. These include:
- Infections – viral or bacterial
- Lack of sleep or tiredness
- Hot environmental temperature: high heat and humidity
- Alcohol
- Spicy food
- Pollen: seasonal exposure in those allergic to pollen
- Hormones: when a person has their period
Exercise may need to be avoided or modified when the above co-factors are present.
For more information on how cofactors affect the risk of anaphylaxis when consuming your food allergen click here.
How much exercise is needed to trigger FDEIA?
With FDEIA, the amount of activity that triggers a reaction may vary.
- Exercise is not necessarily exercise that requires a lot of energy (e.g. running, bike riding, fitness class).
- Some people at risk can develop symptoms from day-to-day activities that require less energy, such as walking, lifting boxes, doing housework (e.g. vacuuming or cleaning), or even rushing to a bus stop, a meeting or back to work from your lunch break.
What are the signs and symptoms of an exercise-induced allergic reaction?
Allergic symptoms may initially appear mild or moderate but can progress rapidly.
However, it is important to remember that mild or moderate allergic symptoms may not always occur before severe symptoms or anaphylaxis.
Signs and symptoms of an allergic reaction
Learn about the signs and symptoms of allergic reactions, and the difference between a mild or moderate reaction and a severe reaction (anaphylaxis).
Diagnosis of FDEIA
FDEIA can be difficult to diagnose, especially if foods other than wheat or seafood are cofactors. People with EIA or FDEIA are sometimes asked to keep a food diary to assist their allergy specialist with identifying a related food trigger. A blood test is often done to help with diagnosis.
When an allergic reaction occurs, write down what happened up to 6 hours before and 4 hours after the allergic reaction (food, drinks, medicines taken and other possible cofactors) or triggers. Make an appointment to speak with your allergy specialist and bring your notes with you.
Daily management of FDEIA or EIA
EIA is a complex condition that should be diagnosed and managed by an allergy specialist. If you are not under the care of one, ask your general practitioner (GP) for a referral.
Management should be individualised (or written specifically for each person) depending on the severity and frequency of symptoms, whether food or cofactors are involved and the desire to play sports or exercise.
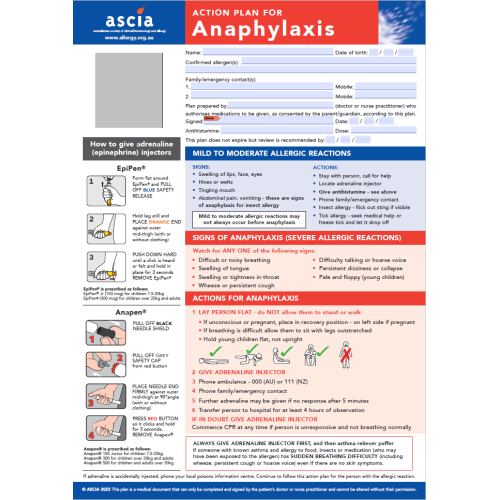
ASCIA Action Plan for Anaphylaxis
The ASCIA Action Plan for Anaphylaxis is for people who have been prescribed an adrenaline (epinephrine) device. It outlines:
- Which allergens to avoid
- Signs of mild to moderate and severe allergic reactions
- Actions to take
- How to give an adrenaline device
- Emergency contact details
The ASCIA Action Plan for Anaphylaxis should be stored with a person’s adrenaline device.
If you have been diagnosed with FDEIA or EIA:
- Be sure to carry your ASCIA Action Plan for Anaphylaxis and your adrenaline (epinephrine) device/s (such as Anapen®, EpiPen®) with you at all times. Have adrenaline easily accessible, including when you are exercising
- Wear a medical identification bracelet or necklace to alert others of the risk of anaphylaxis
- Always read medication labels and avoid NSAIDs, as advised by your doctor
- If you have FDEIA, consider always avoiding the trigger food, not just before/after exercise. Speak with your allergy specialist for advice.
- The reason for this is that occasionally, individuals develop symptoms when food is consumed, and there is little or no exercise at the time of the allergic reaction. So, always read food labels and always disclose your food allergy when eating out.
- If you do choose to eat the trigger food, eat it at a time when you are planning a quiet night at home (such as watching television or reading) with another adult who knows about your allergy and knows that you have eaten the food. Be sure they know what to do in an emergency.
Managing exercise:
- Exercise with a friend or group (who knows about your allergy and your emergency treatment) in case you have an allergic reaction
- Always have your charged phone with you in case you need to call triple zero (000) for an ambulance
- Consider downloading an ‘emergency app’ such as Emergency Plus to your mobile phone so you can call triple zero (000) quickly and the GPS function can let emergency services know where you are.
- Exercise first thing in the morning prior to eating, when possible
- Participate in exercise that can be stopped if necessary, so you don’t ‘push through’ mild symptoms
- Stop exercising at the first sign of symptoms (e.g. extreme tiredness, itch, unexpected redness/flushing, hives)
Is EIA a lifelong condition?
It is not known how long EIA persists or whether it is a condition that people can grow out of.