Updated September 2024
On this page
What is an insect allergy?
An insect allergy is when a person develops symptoms of an allergic reaction after they have been stung or bitten by an insect. Not all reactions to insect bites and stings are the same, some people may develop symptoms of a mild to moderate allergic reaction while others may have a severe allergic reaction (anaphylaxis).
Anaphylaxis to insects is usually due to stinging insects (bees, wasps, ants) as it is the insect venom people are allergic to. Anaphylaxis to biting insects is rare but there have been cases of common bull ants causing anaphylaxis (most allergic reactions to ants are caused by ant stings).
Some biting insects (such as mosquitoes, midges and march flies) can cause large local reactions.
Ticks are not insects but arachnids (same group as spiders) which bite. See our page on Ticks.
Although insects may look similar, allergy to one type of insect does not usually mean the risk of an allergy to another insect is higher.
Stings from insects such as bees, wasps and ants are one of the most common causes of anaphylaxis in Australia.
There are recorded cases of people dying from anaphylaxis following an insect sting. These deaths are usually in older adults with existing lung or heart disease. Death from anaphylaxis remains rare.
Those at greatest risk of anaphylaxis to insects are those who have had anaphylaxis following a sting/bite before.
Common causes of insect allergy
- Honeybee – is the most common cause of allergic reactions to insects in Australia.
- Wasp (Paper wasp and European wasp) – can sting multiple times.
- Jack Jumper Ant (also known as jumper ant or hopper ant) – mostly found in Tasmania, South Australia, Victoria, New South Wales (Snowy Mountains, Blue Mountains and coastal regions), and down the eastern side of Australia.
- Native Australian bees, the red imported fire ant and green ants – can also cause allergic reactions including anaphylaxis.



Signs and symptoms of allergic reactions to insects
Mild to moderate allergic reactions usually settle within a few days.
Signs may include:
- Large local reaction: Rash or swelling around the site of the insect bite or sting.
- Generalised: Some people develop rash/ urticaria (hives) all over their body, without signs or symptoms of anaphylaxis.
People who develop a rash all over their body but do not have signs of anaphylaxis should still be referred to an allergy specialist.
An allergic reaction may start with mild or moderate signs or symptoms but can progress rapidly to anaphylaxis. However, it is important to remember that signs of a mild or moderate allergic reaction may not always occur before anaphylaxis.
Severe allergic reactions to insect sting
Watch for any ONE of these signs of anaphylaxis:
- Difficult or noisy breathing
- Swelling of the tongue
- Swelling or tightness in throat
- Wheeze or persistent cough
- Difficulty talking or hoarse voice
- Persistent dizziness or collapse
- Pale and floppy (young children)
- Abdominal pain, vomiting
With food allergy abdominal pain and vomiting are signs of a mild to moderate allergic reaction. This is because when food you are allergic to is swallowed, your stomach recognises the food protein as dangerous and tries to remove it from your stomach by vomiting. This is different to insect bite and sting allergy where abdominal pain and vomiting are signs of a severe allergic reaction (anaphylaxis). This is because an insect sting or bite can happen anywhere on the body, such as the leg or finger, and the protein from the sting or bite has to travel around the body before it reaches the stomach. When it reaches the stomach and causes abdominal pain and/or vomiting, it means the reaction has spread throughout the body and is no longer a local reaction (that is a reaction in the area of the bite or sting).
Treatment of insect stings/bites
Treatment for a severe allergic reaction (anaphylaxis)
If you have any signs of anaphylaxis, follow the instructions on your ASCIA Action Plan for Anaphylaxis.
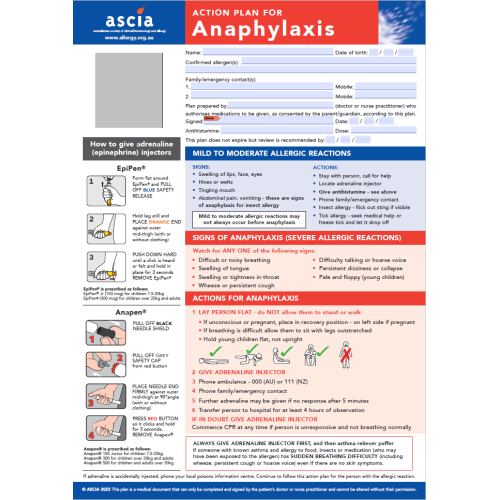
ASCIA Action Plan for Anaphylaxis
The ASCIA Action Plan for Anaphylaxis is for people who have been prescribed an adrenaline (epinephrine) device. It outlines:
- Which allergens to avoid
- Signs of mild to moderate and severe allergic reactions
- Actions to take
- How to give an adrenaline device
- Emergency contact details
The ASCIA Action Plan for Anaphylaxis should be stored with a person’s adrenaline device.
Treatment for large local reactions
- Cold packs may help with itch or hot feeling around the sting/bite.
- Oral antihistamines can help decrease itch.
- Swelling usually goes away in a few days.
See your doctor if the area around the insect sting or bite gets more swollen, redder, hot or more painful, or does not go away within a few days.
Removal of bee stings
- Flicking the stinger out quickly (not squeezing it) may reduce the amount of bee venom injected.
- Use the edge of your fingernail, a car key or credit card to flick out the stinger. For more click here.
Diagnosis of Insect Allergy
People who have had a local reaction such as rash or swelling only near the area of the bite or sting have less than a 10% chance of having a severe allergic reaction (anaphylaxis) to future insect stings or bites.
Insect allergy is more common in adults than children and tends to be lifelong.
The diagnosis of insect allergy should be confirmed by a doctor. This may involve the doctor asking you what happened, a physical examination and they may order some tests. It can help if you know which insect stung/bit you.
If you have had severe allergic reaction (anaphylaxis) from an insect sting/bite, you should ask your doctor for a referral to an allergy specialist. You should also be prescribed an adrenaline device and given an ASCIA Action Plan for Anaphylaxis.
There is treatment available for some types of stinging insect allergy. This is called Venom immunotherapy (VIT) and it has been shown to lessen the severity of allergic reactions in people with insect allergy. VIT needs to be prescribed by an allergy specialist.
To prepare for your allergy specialist appointment read more here.